心源性休克的现有生物标记物和新型生物标记物
IF 16.9
1区 医学
Q1 CARDIAC & CARDIOVASCULAR SYSTEMS
引用次数: 0
摘要
心源性休克(CS)的住院死亡率为30-50%,在过去十年中几乎没有改善。改善预后的挑战与CS的频繁晚期表现或诊断密切相关,因为CS的“不可逆转的点”往往已经过去,导致血流动力学失调,进行性心肌抑制,低血压,低灌注,器官功能障碍和心肌功能下降的螺旋式下降,由炎症和代谢紊乱驱动。根据休克的类型和阶段不同,新的治疗干预措施可能会有不同的疗效。生物标志物有助于预测和早期发现CS,提供器官功能障碍的早期迹象,并确定预后,有助于优化管理。这些生物标志物的时间变化,特别是对药物干预和/或机械循环支持的反应,可以指导管理和预测结果。与乳酸等常规参数相比,一些新的生物标志物增强了对CS死亡率的预测,而肾上腺髓质素和循环二肽基肽酶3等一些生物标志物也能够预测CS的发展。一些生物标志物反映了全身性炎症(如白细胞介素-6、血管生成素2、成纤维细胞生长因子23和致瘤性抑制因子2),并不是CS所特有的,但却提示了参与下行冲击螺旋的重要途径的激活。其他生物标志物信号终末器官灌注不足,可以指导有针对性的干预,而一些可能作为新的治疗靶点。我们严格审查当前和新的生物标志物,指导预测,检测和预测CS。未来使用生物标志物可能有助于改善对这些高危患者的管理。本文章由计算机程序翻译,如有差异,请以英文原文为准。
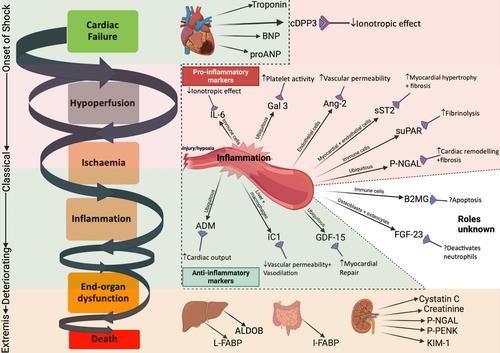
Current and novel biomarkers in cardiogenic shock
Cardiogenic shock (CS) carries a 30–50% in-hospital mortality rate, with little improvement in outcomes in the last decade. Challenges in improving outcomes are closely linked to the frequent late presentation or diagnosis of CS where the ‘point of no return’ has often passed, leading to haemodynamic dysregulation, progressive myocardial depression, hypotension, and a downward spiral of hypoperfusion, organ dysfunction and decreasing myocardial function, driven by inflammation and metabolic derangements. Novel therapeutic interventions may have varying efficacy depending on the type and stage of shock in which they are applied. Biomarkers that aid prediction and early detection of CS, provide early signs of organ dysfunction and define prognosis could help optimize management. Temporal change in such biomarkers, particularly in response to pharmacological interventions and/or mechanical circulatory support, can guide management and predict outcome. Several novel biomarkers enhance the prediction of mortality in CS, compared to conventional parameters such as lactate, with some, such as adrenomedullin and circulating dipeptidyl peptidase 3, also able to predict the development of CS. Some biomarkers reflect systemic inflammation (e.g. interleukin-6, angiopoietin 2, fibroblast growth factor 23 and suppressor of tumorigenicity 2) and are not specific to CS, yet inform on the activation of important pathways involved in the downward shock spiral. Other biomarkers signal end-organ hypoperfusion and could guide targeted interventions, while some may serve as novel therapeutic targets. We critically review current and novel biomarkers that guide prediction, detection, and prognostication in CS. Future use of biomarkers may help improve management in these high-risk patients.
求助全文
通过发布文献求助,成功后即可免费获取论文全文。
去求助
来源期刊

European Journal of Heart Failure
医学-心血管系统
CiteScore
27.30
自引率
11.50%
发文量
365
审稿时长
1 months
期刊介绍:
European Journal of Heart Failure is an international journal dedicated to advancing knowledge in the field of heart failure management. The journal publishes reviews and editorials aimed at improving understanding, prevention, investigation, and treatment of heart failure. It covers various disciplines such as molecular and cellular biology, pathology, physiology, electrophysiology, pharmacology, clinical sciences, social sciences, and population sciences. The journal welcomes submissions of manuscripts on basic, clinical, and population sciences, as well as original contributions on nursing, care of the elderly, primary care, health economics, and other related specialist fields. It is published monthly and has a readership that includes cardiologists, emergency room physicians, intensivists, internists, general physicians, cardiac nurses, diabetologists, epidemiologists, basic scientists focusing on cardiovascular research, and those working in rehabilitation. The journal is abstracted and indexed in various databases such as Academic Search, Embase, MEDLINE/PubMed, and Science Citation Index.
 求助内容:
求助内容: 应助结果提醒方式:
应助结果提醒方式:


