Surgical Management of Deep Brain Stimulator Infection without Electrode Removal: Report of Two Cases.
IF 0.6
Q4 CLINICAL NEUROLOGY
Journal of Neurological Surgery Reports
Pub Date : 2020-01-01
Epub Date: 2020-03-31
DOI:10.1055/s-0039-3399569
引用次数: 2
Abstract
Abstract Objective Stimulation of the subthalamic nucleus by implanted electrodes (deep brain stimulation [DBS]) is performed to suppress symptoms of Parkinson's disease. However, postoperative wound dehiscence and infection can require removal of the implanted electrode leads. This report describes treatment of intractable unilateral wound infection in two patients without removing the DBS device. Methods First, components of the DBS system were removed except for the electrode lead and thorough debridement of the infected wound was conducted. Second, the edges of the bone defect left by removal of DBS components were smoothed to eliminate dead space. Subsequently, the electrode lead was covered by using a pericranial-frontalis-muscle flap or a bi-pedicled-scalp flap with good blood supply. Closed intrawound continuous negative pressure and irrigation treatment was conducted for 1 week after the surgery, and then the drain was removed. Results We treated two patients with wound infection after implantation of DBS electrodes. Case 1 developed a cutaneous fistula and Case 2 had wound dehiscence. After treatment by the method described above, complete wound healing was achieved in both patients. Conclusion DBS is always associated with a risk of infection or exposure of components and treatment can be very difficult. We successfully managed intractable wound infection while leaving the electrode lead in situ, so that it was subsequently possible to continue DBS for Parkinson's disease.
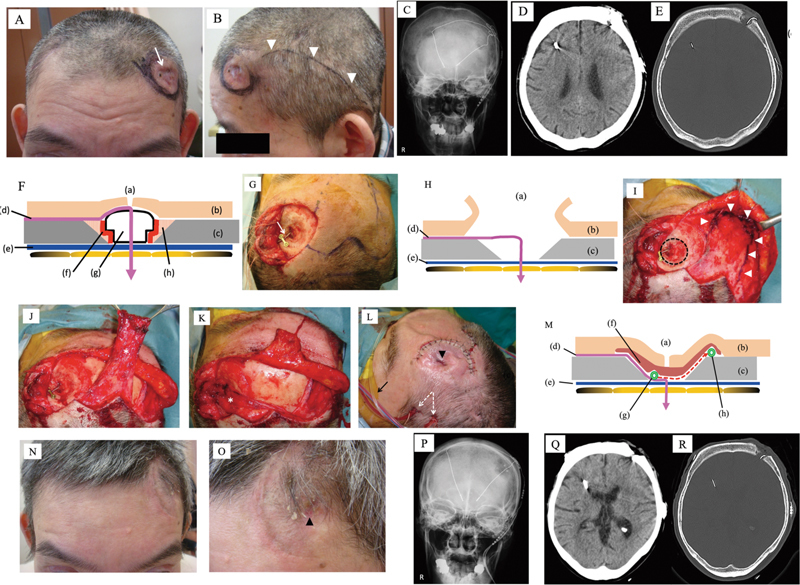
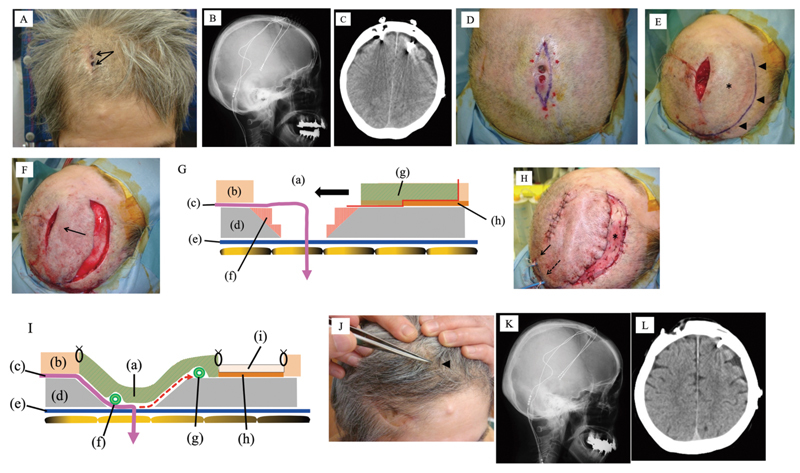
脑深部刺激器感染不切除电极的外科治疗:附2例报告。
目的通过植入电极刺激丘脑下核(深部脑刺激[DBS])来抑制帕金森病的症状。然而,术后伤口裂开和感染可能需要移除植入的电极导线。本报告描述了治疗顽固性单侧伤口感染的两例患者不移除DBS装置。方法首先,除电极引线外,去除DBS系统的其他组成部分,对感染创面进行彻底清创。其次,对移除DBS组件后留下的骨缺损边缘进行平滑处理,消除死区。随后,使用供血良好的颅周-额-肌瓣或双蒂-头皮瓣覆盖电极导线。术后封闭创面内持续负压灌洗1周,拔除引流管。结果我们治疗了2例DBS电极植入后的伤口感染。1例出现皮瘘,2例出现创面裂开。经上述方法治疗后,两例患者伤口均完全愈合。结论DBS总是与感染或暴露成分的风险相关,治疗可能非常困难。我们成功地控制了顽固性伤口感染,同时保留了电极铅,因此随后可以继续对帕金森病进行DBS治疗。
本文章由计算机程序翻译,如有差异,请以英文原文为准。
求助全文
约1分钟内获得全文
求助全文

 求助内容:
求助内容: 应助结果提醒方式:
应助结果提醒方式:


