Continuous Intra-Arterial Blood Pressure Monitoring Improves the Efficiency of Percutaneous Balloon Compression of the Trigeminal Ganglion for Trigeminal Neuralgia.
IF 2.5
3区 医学
Q2 CLINICAL NEUROLOGY
Pain Research & Management
Pub Date : 2022-10-03
eCollection Date: 2022-01-01
DOI:10.1155/2022/7567630
引用次数: 0
Abstract
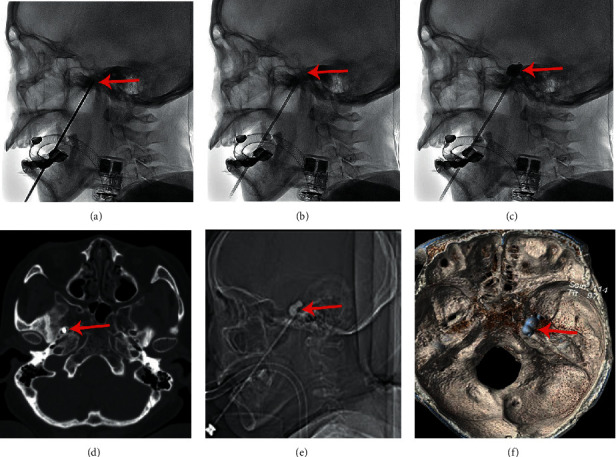
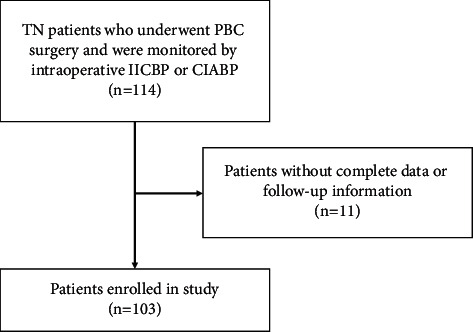
Objective The aim of the study is to explore the characteristics of systolic blood pressure (SBP) and heart rate (HR) changes in patients undergoing percutaneous balloon compression (PBC) for trigeminal neuralgia and analyze the factors that influence the formation of the symbolic pear shape of the balloon, which signifies successful compression. Methods We retrospectively analyzed the changes in systolic blood pressure (SBP) and heart rate (HR) in 103 consecutive patients with trigeminal neuralgia (TN). Fifty-five patients who underwent operations with intermittent inflating cuff blood pressure (IICBP) monitoring were classified into the IICBP group. The other 48 patients who underwent continuous intra-arterial blood pressure (CIABP) monitoring were classified into the CIABP group. Results Among all the patients, there were more women than men and the patients in both the groups more commonly had TN on the right side and involving branch III. First, the balloon appeared as “pear-shaped” when the compression was effective, and the SBP increased an average of 59.04% in the CIABP group. CIABP provided us the precise range of the increase. Older patients had higher SBPs, especially patients with hypertension. Second, SBP was more sensitive and lasted much longer than HR in the process of puncturing the foramen ovale and compressing the ganglion. SBP fluctuated much more in the CIABP group than in the IICBP group. Third, the median time taken in the CIABP group was less than the IICBP group, and the prognosis of the CIABP group was better than the IICBP group. Conclusion Effective ganglion compression significantly increased SBP. CIABP can monitor SBP in real time and can also safeguard the compression process. CIABP is a safe and effective method in the PBC process that is worthy of promotion and application.

持续动脉内血压监测提高经皮球囊压迫三叉神经节治疗三叉神经痛的疗效。
目的:探讨三叉神经痛经皮球囊压迫术(PBC)患者收缩压(SBP)和心率(HR)变化特点,分析影响球囊形成象征压迫成功的梨形的因素。方法:回顾性分析103例三叉神经痛(TN)患者的收缩压(SBP)和心率(HR)的变化。55例接受间歇充气袖带血压(IICBP)监测手术的患者被分为IICBP组。其余48例接受持续动脉内血压(CIABP)监测的患者被分为CIABP组。结果:在所有患者中,女性多于男性,两组患者均以右侧累及III支的TN多见。首先,压缩有效时球囊呈“梨形”,CIABP组收缩压平均升高59.04%。CIABP向我们提供了增长的精确范围。老年患者的sbp较高,尤其是高血压患者。其次,在穿刺卵圆孔压迫神经节的过程中,收缩压比HR更敏感,持续时间更长。与IICBP组相比,CIABP组的收缩压波动更大。第三,CIABP组的中位时间小于IICBP组,且CIABP组的预后优于IICBP组。结论:有效的神经节压迫可显著提高收缩压。CIABP可以实时监测收缩压,并保护压缩过程。CIABP是PBC过程中安全有效的方法,值得推广应用。
本文章由计算机程序翻译,如有差异,请以英文原文为准。
求助全文
约1分钟内获得全文
求助全文
来源期刊

Pain Research & Management
CLINICAL NEUROLOGY-
CiteScore
5.30
自引率
0.00%
发文量
109
审稿时长
>12 weeks
期刊介绍:
Pain Research and Management is a peer-reviewed, Open Access journal that publishes original research articles, review articles, and clinical studies in all areas of pain management.
The most recent Impact Factor for Pain Research and Management is 1.685 according to the 2015 Journal Citation Reports released by Thomson Reuters in 2016.
文献相关原料
| 公司名称 | 产品信息 | 采购帮参考价格 |
|---|
 求助内容:
求助内容: 应助结果提醒方式:
应助结果提醒方式:


