Combined pulsed field ablation and left atrial appendage occlusion: A multicenter comparative study
IF 5.7
2区 医学
Q1 CARDIAC & CARDIOVASCULAR SYSTEMS
引用次数: 0
Abstract
Background
Combining pulsed field ablation (PFA) and left atrial appendage occlusion (LAAO) to 1 procedure is appealing for the treatment of atrial fibrillation.
Objective
This study aimed to compare the outcome of combined and standalone procedures.
Methods
This is a retrospective cohort study of consecutive patients undergoing combined PFA and LAAO procedures in 3 centers in 2023. They underwent PFA pulmonary vein isolation (PVI) with Farapulse (Boston Scientific, Marlborough, MA), followed by LAAO with WATCHMAN FLX (Boston Scientific) guided by transesophageal echocardiogram (TEE). Pulmonary ridge thickness was measured at 45 degrees, 5 mm from tip of the ridge, before and after PFA. At 3 months, TEE or computed tomography was performed for patients with LAAO to assess occlusion results. Peridevice leak (PDL) of more than 3 mm was defined as significant. Consecutive PFA or LAAO standalone procedures served as controls.
Results
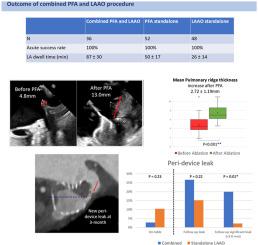
This cohort included 36 combined, 48 standalone LAAO, and 52 standalone PFA cases. Acute PVI was achieved in all combined and PFA standalone procedures. Successful LAAO implantation with WATCHMAN FLX was achieved in 97.2% combined procedures and all standalone LAAO procedures. In the combined cohort, pulmonary ridge thickness increased after ablation by 2.72 ± 1.19 mm (P < .001) or 69.4% ± 51.4%. At 3 months, the rate of PDL did not differ between combined and standalone LAAO cohorts (26.7 vs 15.2%, P = .22). However, significant PDL (> 3 mm) occurred more commonly in the combined cohort compared with the standalone LAAO cohort (20% vs 2.2%, P = .013).
Conclusion
Combined PFA and LAAO was feasible. However, we observed a mean 69.4% increase in pulmonary ridge thickness immediately following PFA. Significant PDL was more prevalent in combined procedure.
联合脉冲场消融与左心耳闭塞——多中心比较研究。
背景:将脉冲场消融(PFA)和左心耳闭塞(LAAO)合并为一种治疗心房颤动的方法是很有吸引力的。目的:比较联合手术和单独手术的结果方法:这是一项回顾性队列研究,研究对象是2023年在3个中心连续接受PFA和LAAO联合手术的患者。采用Farapulse进行PFA肺静脉隔离(PVI),经食管超声心动图(TEE)引导下应用Watchman FLX进行LAAO。在PFA前后,在距脊尖5mm的45度处测量肺脊厚度。在3个月时,对LAAO患者进行TEE或计算机断层扫描以评估闭塞效果。装置周围泄漏(PDL)大于3mm定义为显著。连续的PFA或LAAO独立程序作为对照。结果:该队列包括36例合并病例、48例独立LAAO病例和52例独立PFA病例。急性PVI在所有联合和PFA单独手术中均可实现。Watchman FLX的LAAO植入成功率为97.2%,单独LAAO植入成功率为97.2%。在联合队列中,消融后肺脊厚度增加2.72±1.19mm (p3mm)在联合队列中比单独LAAO队列更常见(20% vs 2.2%, P=0.013)。结论:PFA联合LAAO是可行的。然而,我们观察到PFA后肺脊厚度平均增加69.4%。显著性PDL在联合手术中更为普遍。
本文章由计算机程序翻译,如有差异,请以英文原文为准。
求助全文
约1分钟内获得全文
求助全文
来源期刊

Heart rhythm
医学-心血管系统
CiteScore
10.50
自引率
5.50%
发文量
1465
审稿时长
24 days
期刊介绍:
HeartRhythm, the official Journal of the Heart Rhythm Society and the Cardiac Electrophysiology Society, is a unique journal for fundamental discovery and clinical applicability.
HeartRhythm integrates the entire cardiac electrophysiology (EP) community from basic and clinical academic researchers, private practitioners, engineers, allied professionals, industry, and trainees, all of whom are vital and interdependent members of our EP community.
The Heart Rhythm Society is the international leader in science, education, and advocacy for cardiac arrhythmia professionals and patients, and the primary information resource on heart rhythm disorders. Its mission is to improve the care of patients by promoting research, education, and optimal health care policies and standards.
 求助内容:
求助内容: 应助结果提醒方式:
应助结果提醒方式:


