Best evidence for rehabilitation management of urinary incontinence in patients with bladder cancer following orthotopic neobladder reconstruction
IF 2.8
3区 医学
Q1 NURSING
引用次数: 0
Abstract
Objective
This study aims to establish the best evidence for the rehabilitation management of urinary incontinence (UI) in patients with orthotopic neobladder (ONB) following radical cystectomy (RC) for bladder cancer, providing a theoretical foundation for clinical practice.
Methods
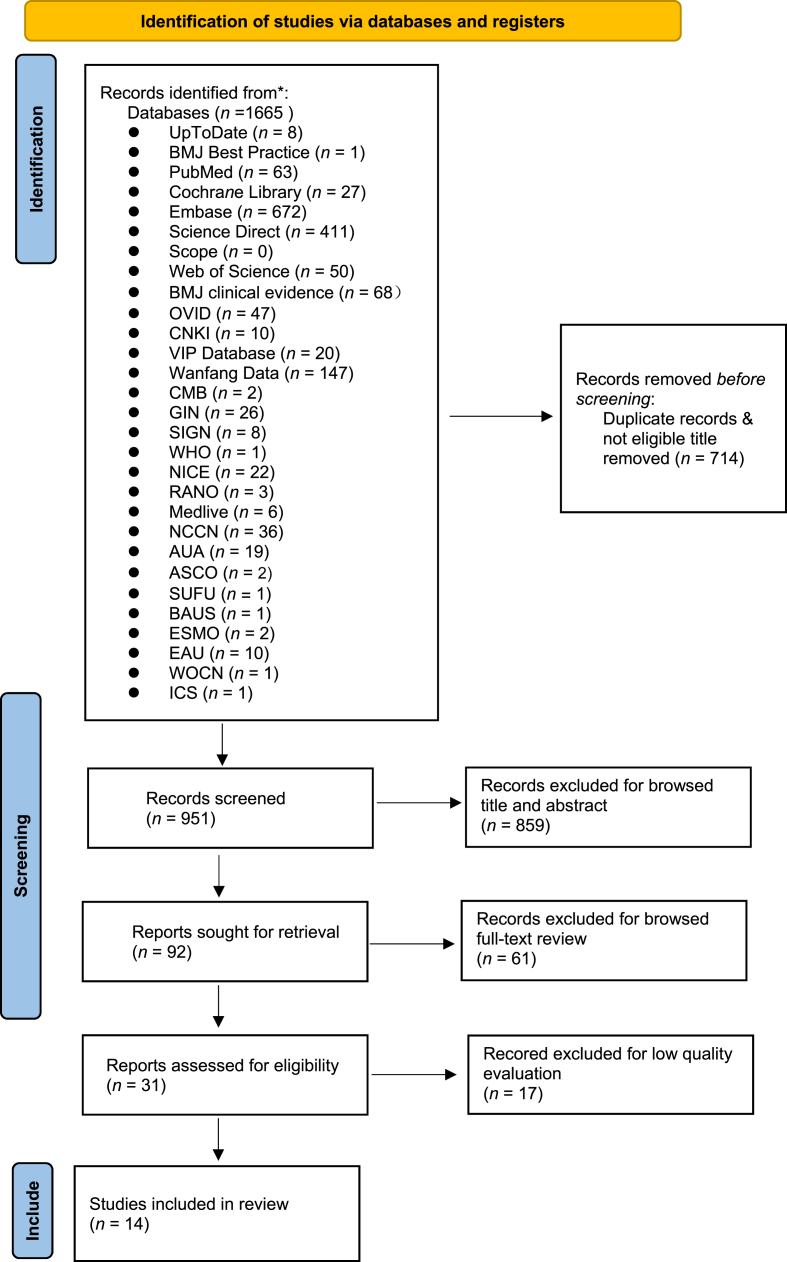
A systematic search was conducted across evidence-based databases, guideline networks, and professional association websites to identify relevant literature on rehabilitation management for patients with ONB after bladder cancer surgery. Studies published in both English and Chinese, up to May 8, 2024, were included. Trained researchers assessed the quality of the literature and summarized the evidence.
Results
Fourteen documents were included, consisting of eight guidelines, two clinical decision documents, and four expert consensus reports. A total of 43 pieces of evidence were identified, covering seven key areas: preoperative UI assessment and counseling, preventive measures, UI assessment and diagnosis, conservative treatments, selection and use of nursing equipment, evaluation of effectiveness, and follow-up care.
Conclusions
The best evidence for UI rehabilitation management after ONB for bladder cancer can help standardize patient care and clinical practices. Healthcare providers should adapt this evidence to their local healthcare settings, cultural contexts, barriers, and patient preferences.
Systematic review registration
This study was conducted following the evidence summary reporting specifications of the Fudan University Center for Evidence-Based Nursing (Registration No. ES20244165).
原位新膀胱重建术后膀胱癌患者尿失禁康复管理的最佳证据。
目的:本研究旨在为膀胱癌根治性膀胱切除术(RC)后原位新膀胱(ONB)患者尿失禁(UI)的康复管理建立最佳证据,为临床实践提供理论基础。方法:系统检索基于证据的数据库、指南网络和专业协会网站,寻找膀胱癌术后ONB患者康复管理的相关文献。截止到2024年5月8日,以中英文发表的研究被纳入其中。训练有素的研究人员评估了文献的质量并总结了证据。结果:共纳入14份文献,包括8份指南、2份临床决策文件和4份专家共识报告。共发现证据43条,涵盖术前尿失速评估与咨询、预防措施、尿失速评估与诊断、保守治疗、护理设备的选择与使用、疗效评价、随访护理等7个重点领域。结论:膀胱癌ONB术后UI康复管理的最佳证据有助于规范患者护理和临床实践。医疗服务提供者应该根据当地的医疗环境、文化背景、障碍和患者偏好来调整这些证据。系统评价注册:本研究遵循复旦大学循证护理研究中心(注册号:ES20244165)。
本文章由计算机程序翻译,如有差异,请以英文原文为准。
求助全文
约1分钟内获得全文
求助全文
来源期刊

Asia-Pacific Journal of Oncology Nursing
Multiple-
CiteScore
2.80
自引率
11.10%
发文量
136
审稿时长
31 days
 求助内容:
求助内容: 应助结果提醒方式:
应助结果提醒方式:


