Illuminating the hidden cost: A systematic review of cognitive late effects regarding cancer-related fatigue in treated paediatric brain tumors
IF 2.8
Q1 Nursing
Technical Innovations and Patient Support in Radiation Oncology
Pub Date : 2024-12-09
DOI:10.1016/j.tipsro.2024.100291
引用次数: 0
Abstract
Objective
Globally, in 2022, 30,871 children were diagnosed with CNS-tumors. Many have been treated with radiotherapy, and a significant number suffer from chronic late effects, including fatigue. This study aims to investigate previous research on the impact of cancer-related fatigue for neurocognitive function that can be related to radiotherapy in patients who have undergone primary brain radiotherapy before the age of 18.
Methods
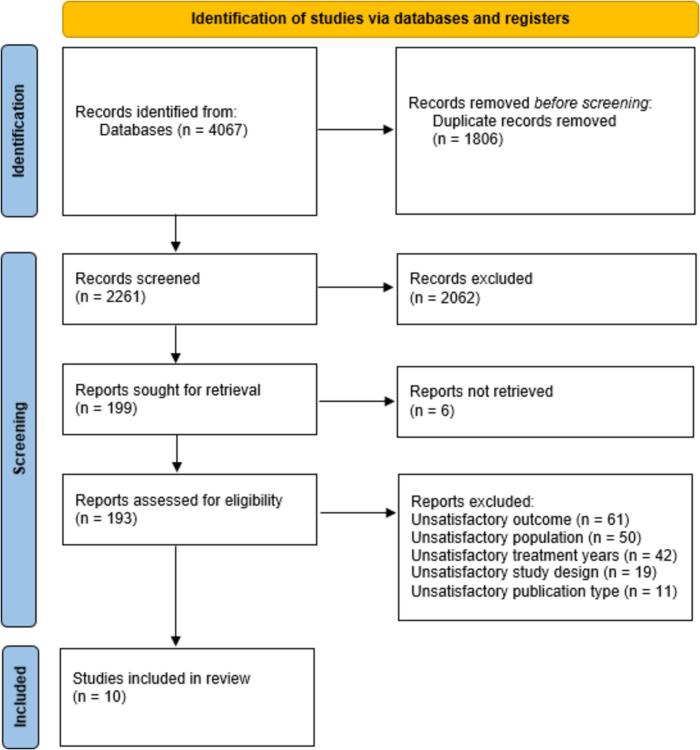
Conducted under PRISMA-S framework, this systematic review searched MEDLINE ALL (Ovid), EMBASE (Ovid), CINAHL (EBSCO), and PsycINFO (Ovid) for relevant studies. Criteria for inclusion were children under 18 who underwent radiotherapy for primary brain cancer, focusing on late cognitive side effects, published 2000–2023.
Results
From 4,067 records, 10 studies were included, examining Proton Radiation Therapy (n = 4), X-ray Radiation Therapy (n = 3), and their comparisons (n = 3). The studies used various cognitive tests, and late effects that emerged were neurocognitive functions and disorders, intellectual functioning, specific cognitive functions and daily life, social functioning, and performance. These themes can be encompassed by cancer-related fatigue.
Conclusions
The findings underscore critical need for more in-depth research to understand the health perception variations among children post-primary brain radiotherapy. Furthermore, detailed insights of treatment specifics, disease progression, target volume sizes, and doses to surrounding organs at risk are imperative.
揭示隐藏的成本:一项关于治疗的儿童脑肿瘤患者癌症相关疲劳的认知晚期效应的系统综述。
目的:在全球范围内,2022年,30,871名儿童被诊断为中枢神经系统肿瘤。许多人接受了放射治疗,而且相当多的人患有慢性晚期症状,包括疲劳。本研究旨在调查18岁之前接受过初级脑放疗的患者的癌症相关性疲劳对神经认知功能的影响,该影响可能与放疗有关。方法:本系统综述在PRISMA-S框架下,检索MEDLINE ALL (Ovid)、EMBASE (Ovid)、CINAHL (EBSCO)和PsycINFO (Ovid)进行相关研究。纳入标准为18岁以下接受原发性脑癌放疗的儿童,重点关注晚期认知副作用,发表于2000-2023年。结果:从4067份记录中,纳入了10项研究,检查了质子放射治疗(n = 4),x射线放射治疗(n = 3)及其比较(n = 3)。这些研究使用了各种认知测试,出现的后期影响包括神经认知功能和障碍、智力功能、特定认知功能和日常生活、社会功能和表现。这些主题可以被癌症相关的疲劳所涵盖。结论:研究结果强调了对儿童原发性脑放疗后健康感知变化进行更深入研究的迫切需要。此外,详细了解治疗细节、疾病进展、靶体积大小和周围器官的风险剂量是必要的。
本文章由计算机程序翻译,如有差异,请以英文原文为准。
求助全文
约1分钟内获得全文
求助全文
来源期刊

Technical Innovations and Patient Support in Radiation Oncology
Nursing-Oncology (nursing)
CiteScore
4.10
自引率
0.00%
发文量
48
审稿时长
67 days
 求助内容:
求助内容: 应助结果提醒方式:
应助结果提醒方式:


