Unilateral-access vs. bilateral-access in transfemoral transcatheter aortic valve replacement: A slim fit approach
IF 3.2
2区 医学
Q2 CARDIAC & CARDIOVASCULAR SYSTEMS
引用次数: 0
Abstract
Background
Vascular complications remain prevalent on transfemoral transcatheter aortic valve replacement (TF-TAVR) with a significant proportion related to the secondary arterial access. We hypothesized that placing the second sheath ipsilateral and distal to the delivery sheath could reduce vascular complications with similar safety and efficacy.
Objectives
Comparing vascular complications and clinical outcomes when placing the secondary arterial sheath in the ipsilateral (unilateral-access) versus in the contralateral (bilateral-access) femoral artery during TF-TAVR.
Methods
Patients who underwent TF-TAVR using unilateral-access as first-choice approach were retrospectively compared with a contemporaneous bilateral-access group. The primary endpoint was the incidence of vascular complications related to femoral access according to the VARC-3 criteria. A propensity-score analysis was performed accounting for the differences in clinical, vascular, and procedural characteristics.
Results
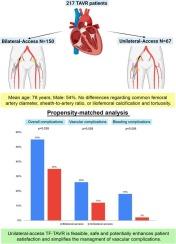
A total of 217 patients were included, of whom 150 (69.1 %) underwent TF-TAVR through bilateral- and 67 (30.9 %) through unilateral-access. Vascular complications occurred in 16.0 % of the bilateral-access group and 10.4 % of the unilateral-access group (p = 0.280). The unilateral-access group achieved high procedural success with normalization of peak aortic velocity and low rates of paravalvular leaks, valve migration and pacemaker requirement. After propensity-score matching, the overall complications rate was superior in the bilateral-access group (54.4 % vs 35.1 %, p = 0.038) due to a trend of higher vascular complications (26.3 % vs 12.3 %, p = 0.058) and a significant higher occurrence of bleeding complications (17.5 % vs 1.8 %, p = 0.008).
Conclusions
Unilateral-access TF-TAVR is feasible, safe, and potentially enhances procedural efficiency and patient satisfaction while maintaining the capacity for bailout interventions in managing vascular complications.
经股动脉经导管主动脉瓣置换术中的单侧入路与双侧入路:纤细贴合方法。
背景:经口经导管主动脉瓣置换术(TF-TAVR)的血管并发症仍然很普遍,其中很大一部分与二次动脉通路有关。我们假设,在输送鞘的同侧和远端放置第二根鞘可减少血管并发症,同时具有相似的安全性和有效性:比较在 TF-TAVR 期间将第二动脉鞘放置在同侧(单侧入路)与对侧(双侧入路)股动脉时的血管并发症和临床结果:回顾性比较了以单侧入路为首选方法进行TF-TAVR的患者和同时进行双侧入路手术的患者。根据 VARC-3 标准,主要终点是与股骨入路相关的血管并发症发生率。考虑到临床、血管和手术特征的差异,进行了倾向分数分析:共纳入217名患者,其中150人(69.1%)通过双侧入路接受了TF-TAVR,67人(30.9%)通过单侧入路接受了TF-TAVR。双侧入路组发生血管并发症的比例为 16.0%,单侧入路组为 10.4%(P = 0.280)。单侧入路组手术成功率高,主动脉峰值速度正常,瓣膜旁漏、瓣膜移位和起搏器需求率低。经过倾向分数匹配后,双侧入路组的总体并发症发生率更高(54.4% vs 35.1%,p = 0.038),原因是血管并发症呈上升趋势(26.3% vs 12.3%,p = 0.058),出血并发症的发生率也明显更高(17.5% vs 1.8%,p = 0.008):单侧入路 TF-TAVR 是可行的、安全的,有可能提高手术效率和患者满意度,同时在处理血管并发症时保持救助干预能力。
本文章由计算机程序翻译,如有差异,请以英文原文为准。
求助全文
约1分钟内获得全文
求助全文
来源期刊

International journal of cardiology
医学-心血管系统
CiteScore
6.80
自引率
5.70%
发文量
758
审稿时长
44 days
期刊介绍:
The International Journal of Cardiology is devoted to cardiology in the broadest sense. Both basic research and clinical papers can be submitted. The journal serves the interest of both practicing clinicians and researchers.
In addition to original papers, we are launching a range of new manuscript types, including Consensus and Position Papers, Systematic Reviews, Meta-analyses, and Short communications. Case reports are no longer acceptable. Controversial techniques, issues on health policy and social medicine are discussed and serve as useful tools for encouraging debate.
 求助内容:
求助内容: 应助结果提醒方式:
应助结果提醒方式:


