The prognostic significance of diabetes in non-small cell lung cancer patients treated with immune checkpoint inhibitors: A meta-analysis
IF 6.1
3区 医学
Q1 ENDOCRINOLOGY & METABOLISM
引用次数: 0
Abstract
Aims
Studies on the prognosis of patients with diabetes and non-small-cell lung cancer (NSCLC) in the era of immune checkpoint inhibitors (ICIs) are limited, and existing findings remain inconsistent. This meta-analysis explored the association between diabetes and survival outcomes in this population.
Methods
A total of 10 non-randomized studies comparing overall survival between patients with NSCLC receiving ICIs with and without diabetes were included. A meta-analysis was performed to estimate the hazard of death or disease progression between the two groups. Another analysis was employed to explore the difference in median survival between the groups. Additionally, subgroup, meta-regression, and sensitivity analyses were conducted.
Results
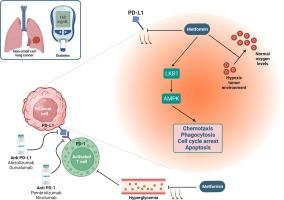
Patients with diabetes exhibited a significantly higher risk of death than those without diabetes (HR = 1.28, 95 % CI = 1.14–1.44; P < 0.01). Moreover, individuals with diabetes had a median life expectancy that was 6.04 months shorter (95 % CI = −10.53 to − 1.54 months, P = 0.009) than that of individuals without diabetes. Moreover, for every 1 % increase in the proportion of patients with diabetes using metformin, a corresponding 2.2 % decrease in the HR of progression-free survival was observed (95 % CI = 1.2–3.1 %).
Conclusion
Diabetes compromises the effectiveness of ICI treatment in patients with NSCLC.
接受免疫检查点抑制剂治疗的非小细胞肺癌患者中糖尿病的预后意义:荟萃分析
目的:在使用免疫检查点抑制剂(ICIs)的时代,有关糖尿病和非小细胞肺癌(NSCLC)患者预后的研究十分有限,现有研究结果仍不一致。这项荟萃分析探讨了糖尿病与该人群生存结果之间的关联:方法:共纳入了 10 项非随机研究,比较了接受 ICIs 治疗的 NSCLC 患者患糖尿病和未患糖尿病的总生存率。我们进行了一项荟萃分析,以估算两组患者的死亡或疾病进展风险。另一项分析用于探讨两组患者中位生存期的差异。此外,还进行了亚组、元回归和敏感性分析:结果:糖尿病患者的死亡风险明显高于非糖尿病患者(HR = 1.28,95 % CI = 1.14-1.44;P 结论:糖尿病会影响 IC 治疗的效果:糖尿病会影响 ICI 对 NSCLC 患者的治疗效果。
本文章由计算机程序翻译,如有差异,请以英文原文为准。
求助全文
约1分钟内获得全文
求助全文
来源期刊

Diabetes research and clinical practice
医学-内分泌学与代谢
CiteScore
10.30
自引率
3.90%
发文量
862
审稿时长
32 days
期刊介绍:
Diabetes Research and Clinical Practice is an international journal for health-care providers and clinically oriented researchers that publishes high-quality original research articles and expert reviews in diabetes and related areas. The role of the journal is to provide a venue for dissemination of knowledge and discussion of topics related to diabetes clinical research and patient care. Topics of focus include translational science, genetics, immunology, nutrition, psychosocial research, epidemiology, prevention, socio-economic research, complications, new treatments, technologies and therapy.
 求助内容:
求助内容: 应助结果提醒方式:
应助结果提醒方式:


