Impact of Neighborhood Disadvantage on Preventive and Acute Care Utilization in Sickle Cell Disease
Abstract
Background
Individuals with sickle cell disease (SCD) experience significant healthcare disparities; however, there is little known on the impact of psychosocial stressors and neighborhood disadvantage on preventive and acute care utilization in this population.
Procedure
A retrospective data collection was performed for all patients cared for at a comprehensive pediatric sickle cell center in the Midwest who had also completed the Psychosocial Assessment Tool (PAT), a validated caregiver-reported measurement of family psychosocial risk, from September 2021 through December 2022. Patient age, payor, primary language, frequency of acute and missed preventive care visits, as well as Area Deprivation Index (ADI) and Childhood Opportunity Index (COI) scores were collected for 256 patients.
Results
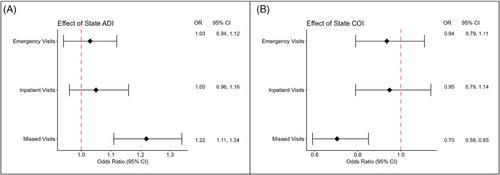
The average state ADI was 6.3 (±2.9), and the majority of patients were in the Very Low or Low COI categories. Total PAT score (p = 0.003), state ADI (p < 0.001), and state COI (p < 0.001) were all significantly correlated with missed SCD clinic visits, with increased odds of a missed visit with increasing neighborhood disadvantage (OR 1.22, p < 0.001). The odds of acute care were also increased in those with higher family psychosocial risk (OR 1.76, p < 0.011), though this was not seen with ADI or COI, suggesting an additional effect of family stressors and resilience on acute care utilization.
Conclusions
This highlights the importance of regular, universal social and psychological risk screening, as well as inclusion of psychosocial team members in SCD programs to identify and readily address risk factors that impact child outcomes in a minoritized chronic disease population.

 求助内容:
求助内容: 应助结果提醒方式:
应助结果提醒方式:


