Clinical Risk Factors for High-Dose Methotrexate-Induced Oral Mucositis Following Individualized Dosing
Abstract
Background
Oral mucositis affects about 20% of children undergoing high-dose methotrexate (HDMTX) for acute lymphoblastic leukemia (ALL), despite existing management strategies. Personalized HDMTX dosing, adjusted by pharmacokinetics and leukemia risk, has reduced mucositis incidence, but variations still occur with similar 24-h methotrexate levels.
Methods
This retrospective study investigated risk factors for oral mucositis under individualized methotrexate protocols. Data from patients with ≥ Grade 2 oral mucositis (CTCAE v4.0) were analyzed from the St. Jude Children's Research Hospital total 16 trial. A 1:1 case–control matching method considered age, sex, risk classification, immunophenotype, and methotrexate course. McNemar's, Bowker's symmetry, and Wilcoxon signed-rank tests were used for statistical analyses. Risk factors for recurrent mucositis were identified in a case-only analysis.
Results
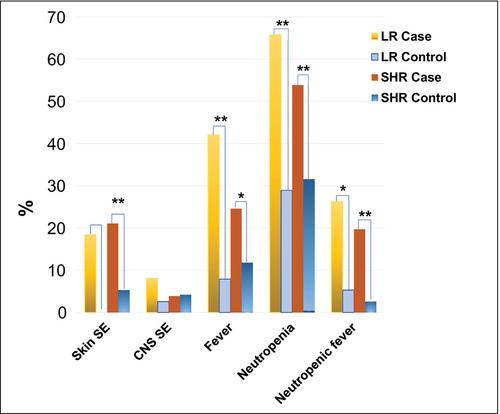
The study found significant associations between methotrexate-induced mucositis and new-onset skin rashes (p = 0.0027), fever (p = 0.0016), neutropenic fever (p = 0.0008), lower absolute neutrophil count (p < 0.0001), acute kidney injury (AKI) (p = 0.0164), delayed methotrexate clearance (p = 0.0133), and higher 42-h methotrexate levels (p = 0.0179). In the standard/high-risk group, mercaptopurine dose was also linked to mucositis (p = 0.0495). Multivariable analysis showed that skin rashes (OR 6.5, p = 0.0016), fever (OR 2.8, p = 0.009), and neutropenia (OR 2.3, p = 0.0106) were independent risk factors for mucositis. Female sex (OR 7.12, p = 0.015) and AKI (OR 3.819, p = 0.037) were associated with recurrent mucositis.
Conclusions
Fever, skin rashes, AKI, delayed methotrexate clearance, and higher 42-h methotrexate levels were key risk factors for HDMTX-induced oral mucositis. Skin rashes, fever, and neutropenia were independent predictors, while female sex and AKI were linked to recurrent mucositis.
 求助内容:
求助内容: 应助结果提醒方式:
应助结果提醒方式:


