Association Between Organizational Context and Resident Pain in Assisted Living: A Repeated Cross-Sectional Study
Abstract
Objectives
Resident pain has been a common quality challenge in congregate care for older adults, and organizational context may explain variations in resident pain beyond resident-level factors. Most studies have focused on nursing homes (NHs), largely neglecting assisted living (AL). AL residents are at similar risk for pain as NH resident, but with AL providing fewer services and staffing resources. Our objective was to examine whether organizational context in AL was associated with resident pain during the first two waves of the COVID-19 pandemic.
Methods
This repeated cross-sectional study linked AL home surveys, collected in COVID-19 waves 1 (March–June 2020) and 2 (October 2020–February 2021) from a key contact, to administrative Resident Assessment Instrument-Home Care (RAI-HC) records in these homes. Surveys assessed preparedness for COVID-19 outbreaks, availability of a registered nurse or nurse practitioner, direct care staff shortages, decreased staff morale, COVID-19 outbreaks, confinement of residents to their rooms, supporting video calls with physicians, facilitating caregiver involvement. The dependent variable (moderate daily pain or pain of a severe intensity) and resident covariates came from the RAI-HC. Using general estimating equations, adjusted for repeated resident assessments and covariates, we assessed whether AL organizational context was associated with resident pain during the pandemic.
Results
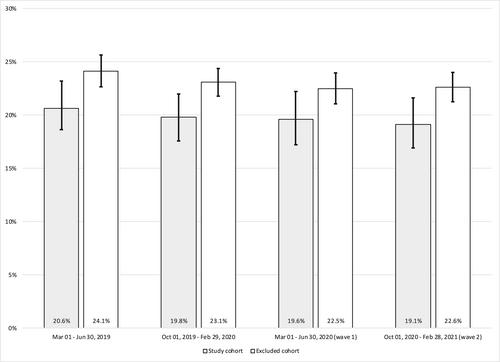
We included 985 residents in 41 facilities (wave 1), and 1134 residents in 42 facilities (wave 2). Pain prevalence [95% confidence interval] decreased non-significantly from 20.6% [18.6%–23.2%] (March–June 2019) to 19.1% [16.9%–21.6%] (October 2020–February 2021). Better preparedness (odds ratio = 1.383 [1.025–1.866]), confinement of residents to their rooms (OR = 1.616 [1.212–2.155]), availability of a nurse practitioner (OR = 0.761 [0.591–0.981]), and staff shortages (OR = 0.684 [0.527–0.888]) were associated with resident pain.
Conclusions
AL organizational context factors were associated with resident pain. Policy and management interventions can and must address such factors, providing potentially powerful levers for improving AL resident quality of care.

 求助内容:
求助内容: 应助结果提醒方式:
应助结果提醒方式:


