Blood markers for type-1,-2, and -3 inflammation are associated with severity of acutely decompensated cirrhosis
IF 26.8
1区 医学
Q1 GASTROENTEROLOGY & HEPATOLOGY
引用次数: 0
Abstract
Background and aims
In patients with acutely decompensated cirrhosis (ADC) who present with clinically apparent precipitants (i.e., infections, acute liver injury), alterations in blood markers of inflammation associate with progression toward severe phenotypes (e.g., acute-on-chronic liver failure, ACLF). It is unclear whether alterations in blood inflammatory markers may associate with progression of ADC independently of precipitants.Methods
We prospectively enrolled 394 patients admitted for ADC who were classified into four phenotypes of increasing severity: no organ dysfunction (n=168), organ dysfunction alone (n=72), organ failure without ACLF (n=91), and ACLF (n=63). Clinical blood cell counts and serum levels of inflammatory markers (including soluble markers related to type-1, type-2, and type-3 inflammation) were obtained at enrollment. Ordinal regression with adjacent categories logit model adjusted for confounders (including precipitants) was used to analyze associations between changes in each blood inflammatory marker and the worsening of ADC.Results
Inflammatory markers that were associated with higher risk of progressing to the next more severe stage were as follows: increasing neutrophil counts (adjusted common odds ratio [cOR] 1.17, 95%CI 1.06-1.28); increasing levels of the type-2 cytokine interleukin (IL)-25 (cOR 1.21, 95%CI 1.06-1.39), type-3 cytokines IL-6 (cOR 1.15, 95%CI 1.02-1.28) and IL-22 (cOR 1.16, 95%CI 1.03-1.30), or anti-inflammatory soluble CD163 (cOR 1.94, 95%CI 1.58-2.38); decreasing lymphocyte counts (cOR 0.77, 95%CI 0.68-0.87), or decreasing levels of the type-1 cytokine IFN-γ (cOR 0.85, 95%CI 0.75-0.95).Conclusions
Among patients with ADC, alterations in blood levels of cytokines related to type-1, type-2 and type-3 inflammation, together with neutrophilia, lymphopenia and elevated anti-inflammatory signals were individually associated with an increased risk of progressing toward ACLF, independently of the presence of clinically apparent precipitants.
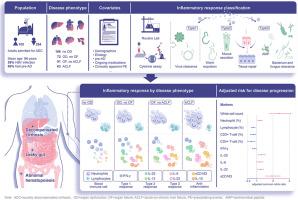
1、2 和 3 型炎症的血液标记物与急性失代偿期肝硬化的严重程度有关
背景和目的在临床上有明显诱因(如感染、急性肝损伤)的急性失代偿性肝硬化(ADC)患者中,血液炎症标志物的改变与向严重表型(如急性-慢性肝衰竭,ACLF)的进展有关。目前还不清楚血液中炎症标志物的改变是否与 ADC 的进展无关。方法我们前瞻性地纳入了 394 例因 ADC 入院的患者,这些患者被分为四种严重程度依次递增的表型:无器官功能障碍(168 例)、单纯器官功能障碍(72 例)、无 ACLF 的器官衰竭(91 例)和 ACLF(63 例)。临床血细胞计数和血清炎症标志物水平(包括与1型、2型和3型炎症相关的可溶性标志物)均在入组时获得。采用调整了混杂因素(包括诱发因素)的邻近类别对数模型进行顺序回归,分析每种血液炎症标记物的变化与 ADC 恶化之间的关系。结果与进展到下一个更严重阶段的更高风险相关的炎症标志物如下:中性粒细胞计数增加(调整后的共同几率比 [cOR] 1.17,95%CI 1.06-1.28);2型细胞因子白细胞介素(IL)-25(cOR 1.21,95%CI 1.06-1.39)、3型细胞因子IL-6(cOR 1.15,95%CI 1.02-1.28)和IL-22(cOR 1.16,95%CI 1.03-1.30),或抗炎可溶性 CD163(cOR 1.94,95%CI 1.58-2.38);淋巴细胞计数减少(cOR 0.77,95%CI 0.68-0.87),或 1 型细胞因子 IFN-γ 水平下降(cOR 0.85,95%CI 0.75-0.95)。结论在 ADC 患者中,血液中与 1 型、2 型和 3 型炎症相关的细胞因子水平的改变,以及中性粒细胞增多、淋巴细胞减少和抗炎信号升高,均与进展为 ACLF 的风险增加有关,与临床上明显的诱因无关。
本文章由计算机程序翻译,如有差异,请以英文原文为准。
求助全文
约1分钟内获得全文
求助全文
来源期刊

Journal of Hepatology
医学-胃肠肝病学
CiteScore
46.10
自引率
4.30%
发文量
2325
审稿时长
30 days
期刊介绍:
The Journal of Hepatology is the official publication of the European Association for the Study of the Liver (EASL). It is dedicated to presenting clinical and basic research in the field of hepatology through original papers, reviews, case reports, and letters to the Editor. The Journal is published in English and may consider supplements that pass an editorial review.
 求助内容:
求助内容: 应助结果提醒方式:
应助结果提醒方式:


