Real-world data on ALK rearrangement test in Chinese advanced non-small cell lung cancer (RATICAL): a nationwide multicenter retrospective study
Abstract
Background
Anaplastic lymphoma kinase (ALK) test in advanced non-small cell lung cancer (NSCLC) can help physicians provide target therapies for patients harboring ALK gene rearrangement. This study aimed to investigate the real-world test patterns and positive rates of ALK gene rearrangements in advanced NSCLC.
Methods
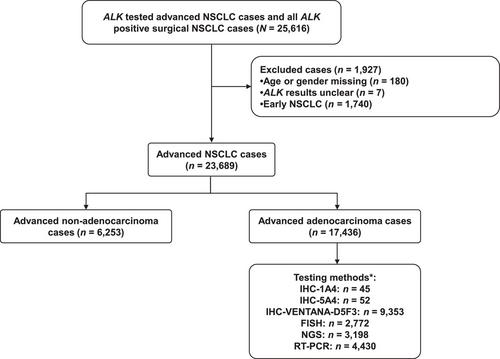
In this real-world study (ChiCTR2000030266), patients with advanced NSCLC who underwent an ALK rearrangement test in 30 medical centers in China between October 1, 2018 and December 31, 2019 were retrospectively analyzed. Interpretation training was conducted before the study was initiated. Quality controls were performed at participating centers using immunohistochemistry (IHC)-VENTANA-D5F3. The positive ALK gene rearrangement rate and consistency rate were calculated. The associated clinicopathological characteristics of ALK gene rearrangement were investigated as well.
Results
The overall ALK gene rearrangement rate was 6.7% in 23,689 patients with advanced NSCLC and 8.2% in 17,436 patients with advanced lung adenocarcinoma. The quality control analysis of IHC-VENTANA-D5F3 revealed an intra-hospital consistency rate of 98.2% (879/895) and an inter-hospital consistency rate of 99.2% (646/651). IHC-VENTANA-D5F3 was used in 53.6%, real-time polymerase chain reaction (RT-PCR) in 25.4%, next-generation sequencing (NGS) in 18.3%, and fluorescence in-situ hybridization (FISH) in 15.9% in the adenocarcinoma subgroup. For specimens tested with multiple methods, the consistency rates confirmed by IHC-VENTANA-D5F3 were 98.0% (822/839) for FISH, 98.7% (1,222/1,238) for NGS, and 91.3% (146/160) for RT-PCR. The overall ALK gene rearrangement rates were higher in females, patients of ≤ 35 years old, never smokers, tumor cellularity of > 50, and metastatic specimens used for testing in the total NSCLC population and adenocarcinoma subgroup (all P < 0.05).
Conclusions
This study highlights the real-world variability and challenges of ALK test in advanced NSCLC, demonstrating a predominant use of IHC-VENTANA-D5F3 with high consistency and distinct clinicopathological features in ALK-positive patients. These findings underscore the need for a consensus on optimal test practices and support the development of refined ALK test strategies to enhance diagnostic accuracy and therapeutic decision-making in NSCLC.

 求助内容:
求助内容: 应助结果提醒方式:
应助结果提醒方式:


