Mediterranean-style dietary interventions in adults with cancer: a systematic review of the methodological approaches, feasibility, and preliminary efficacy
IF 3.6
3区 医学
Q2 NUTRITION & DIETETICS
引用次数: 0
Abstract
Cancer and its treatments can lead to excess body fat, decreases in lean mass, cardiotoxicity, and other side effects. The Mediterranean diet (MED-diet) has the potential to improve clinical and supportive care outcomes. The aim of this systematic review was to evaluate the feasibility, safety, and efficacy of the MED-diet on health outcomes in adults with cancer. Three databases were searched from inception to February 2023. Eligible studies included randomised controlled trials testing a MED-diet intervention among adults with cancer. Within- and between-group differences for adherence, dietary intake and health outcomes were extracted. Fifteen studies describing fourteen interventions were included, and there were considerable differences in study design and implementation of the MED-diet. Studies were predominately in women with a history of breast cancer. The MED-diet was safe with no adverse events reported, and feasible with high adherence and/or increases in MED-diet-compliant foods. The MED-diet when applied with an energy restriction below estimated requirements for weight loss demonstrated reductions in body weight (range: −3.9 kg to −0.7 kg). Interventions that showed significant reductions in body weight also improved quality of life. There is limited evidence to evaluating the MED-diet on cardiovascular and inflammatory markers, and heterogenous MED-diet prescriptions impede definitive conclusions on these health outcomes. The MED-diet was feasible and safe for adults with cancer. There were reported benefits for weight loss following a MED-diet when an energy restriction was applied, however further evaluation to determine the effects on cardiometabolic biomarkers and other outcomes are required.
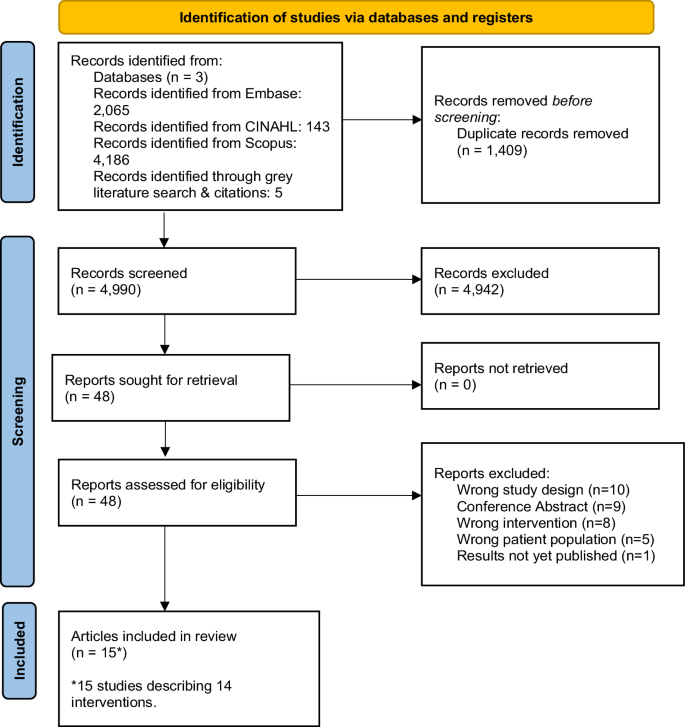
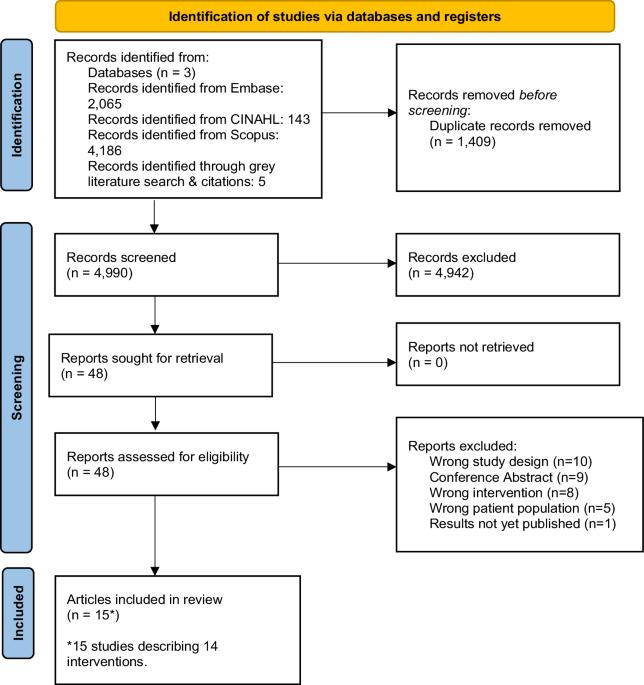
对成人癌症患者进行地中海式饮食干预:对方法、可行性和初步疗效的系统回顾。
背景:癌症及其治疗会导致体内脂肪过多、瘦肉减少、心脏毒性和其他副作用。地中海饮食(MED-diet)具有改善临床和支持性治疗效果的潜力。本系统性综述旨在评估地中海饮食对成人癌症患者健康结果的可行性、安全性和有效性:方法:检索了从开始到 2023 年 2 月的三个数据库。符合条件的研究包括在成年癌症患者中测试 MED 饮食干预的随机对照试验。结果:15 项研究描述了 14 种饮食干预方法:结果:共纳入了 15 项研究,描述了 14 项干预措施,研究设计和 MED 饮食的实施存在很大差异。研究对象主要是有乳腺癌病史的妇女。MED 饮食法是安全的,没有不良事件的报道,而且在坚持率高和/或增加符合 MED 饮食法的食物的情况下是可行的。MED 饮食法的能量限制低于减肥的估计要求,可减轻体重(范围:-3.9 千克至-0.7 千克)。体重明显减轻的干预措施也改善了生活质量。评估 MED 饮食对心血管和炎症指标影响的证据有限,而且不同的 MED 饮食处方阻碍了对这些健康结果得出明确结论:结论:MED 饮食法对成年癌症患者是可行和安全的。据报道,在限制能量摄入的情况下,采用 MED 饮食法可以减轻体重,但还需要进一步评估其对心血管代谢生物标志物和其他结果的影响。
本文章由计算机程序翻译,如有差异,请以英文原文为准。
求助全文
约1分钟内获得全文
求助全文
来源期刊
CiteScore
10.60
自引率
2.10%
发文量
189
审稿时长
3-6 weeks
期刊介绍:
The European Journal of Clinical Nutrition (EJCN) is an international, peer-reviewed journal covering all aspects of human and clinical nutrition. The journal welcomes original research, reviews, case reports and brief communications based on clinical, metabolic and epidemiological studies that describe methodologies, mechanisms, associations and benefits of nutritional interventions for clinical disease and health promotion.
Topics of interest include but are not limited to:
Nutrition and Health (including climate and ecological aspects)
Metabolism & Metabolomics
Genomics and personalized strategies in nutrition
Nutrition during the early life cycle
Health issues and nutrition in the elderly
Phenotyping in clinical nutrition
Nutrition in acute and chronic diseases
The double burden of ''malnutrition'': Under-nutrition and Obesity
Prevention of Non Communicable Diseases (NCD)

 求助内容:
求助内容: 应助结果提醒方式:
应助结果提醒方式:


