Time to blood pressure control and predictors among patients receiving integrated treatment for hypertension and HIV based on an adapted WHO HEARTS implementation strategy at a large urban HIV clinic in Uganda
IF 2.7
4区 医学
Q2 PERIPHERAL VASCULAR DISEASE
引用次数: 0
Abstract
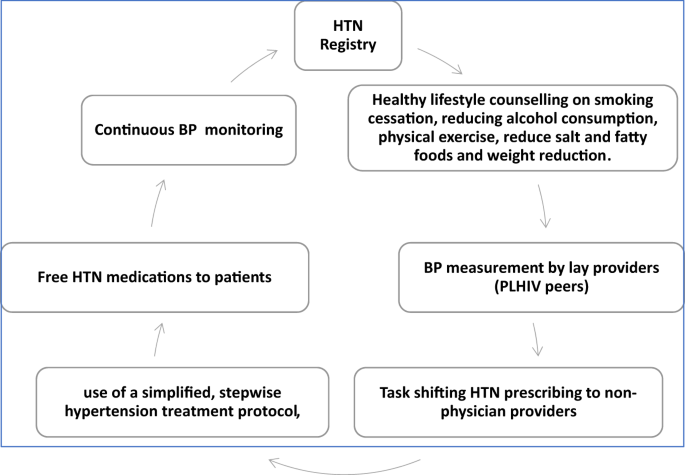
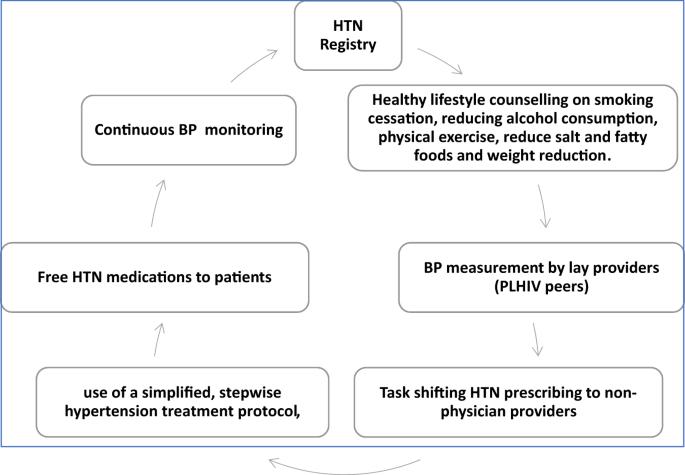
In this cohort study, we determined time to blood pressure (BP) control and its predictors among hypertensive PLHIV enrolled in integrated hypertension-HIV care based on the World Health Organization (WHO) HEARTS strategy at Mulago Immunosuppression Clinic in Uganda. From August 2019 to March 2020, we enrolled hypertensive PLHIV aged $$\ge$$ 18 years and initiated Amlodipine 5 mg mono-therapy for BP (140–159)/(90–99) mmHg or Amlodipine 5 mg/Valsartan 80 mg duo-therapy for BP ≥ 160/90 mmHg. Patients were followed with a treatment escalation plan until BP control, defined as BP < 140/90 mmHg. We used Cox proportional hazards models to identify predictors of time to BP control. Of 877 PLHIV enrolled (mean age 50.4 years, 62.1% female), 30% received mono-therapy and 70% received duo-therapy. In the monotherapy group, 66%, 88% and 96% attained BP control in the first, second and third months, respectively. For patients on duo-therapy, 56%, 83%, 88% and 90% achieved BP control in the first, second, third, and fourth months, respectively. In adjusted Cox proportional hazard analysis, higher systolic BP (aHR 0.995, 95% CI 0.989-0.999) and baseline ART tenofovir/lamivudine/efavirenz (aHR 0.764, 95% CI 0.637–0.917) were associated with longer time to BP control, while being on ART for >10 years was associated with a shorter time to BP control (aHR 1.456, 95% CI 1.126–1.883). The WHO HEARTS strategy was effective at achieving timely BP control among PLHIV. Additionally, monotherapy anti-hypertensive treatment for stage I hypertension is a viable option to achieve BP control and limit pill burden in resource limited HIV care settings.
乌干达一家大型城市艾滋病毒诊所根据经过调整的世界卫生组织 HEARTS 实施战略,对接受高血压和艾滋病毒综合治疗的患者进行血压控制的时间和预测因素
在这项队列研究中,我们确定了乌干达穆拉戈免疫抑制诊所根据世界卫生组织(WHO)HEARTS战略开展的高血压-艾滋病毒综合护理中高血压PLHIV的血压(BP)控制时间及其预测因素。从2019年8月至2020年3月,我们招募了年龄为18岁的高血压PLHIV,并对血压为(140-159)/(90-99)mmHg的患者采用氨氯地平5毫克单药治疗,或对血压≥160/90mmHg的患者采用氨氯地平5毫克/缬沙坦80毫克双药治疗。按照治疗升级计划对患者进行随访,直至血压控制(定义为血压< 140/90 mmHg)。我们使用 Cox 比例危险模型来确定血压控制时间的预测因素。在登记的 877 名艾滋病毒感染者(平均年龄 50.4 岁,62.1% 为女性)中,30% 接受了单一疗法,70% 接受了双重疗法。在单一疗法组中,分别有 66%、88% 和 96% 的患者在第一、第二和第三个月达到了血压控制。在接受双重疗法的患者中,分别有 56%、83%、88% 和 90% 的患者在第一、第二、第三和第四个月实现了血压控制。在调整后的 Cox 比例危险分析中,较高的收缩压(aHR 0.995,95% CI 0.989-0.999)和基线抗逆转录病毒疗法替诺福韦/拉米夫定/依非韦伦(aHR 0.764,95% CI 0.637-0.917)与较长的血压控制时间相关,而接受抗逆转录病毒疗法 10 年与较短的血压控制时间相关(aHR 1.456,95% CI 1.126-1.883)。世卫组织的 HEARTS 策略能有效地使 PLHIV 患者及时控制血压。此外,在资源有限的艾滋病护理环境中,I期高血压的单药抗高血压治疗是实现血压控制和限制药片负担的可行选择。
本文章由计算机程序翻译,如有差异,请以英文原文为准。
求助全文
约1分钟内获得全文
求助全文
来源期刊

Journal of Human Hypertension
医学-外周血管病
CiteScore
5.20
自引率
3.70%
发文量
126
审稿时长
6-12 weeks
期刊介绍:
Journal of Human Hypertension is published monthly and is of interest to health care professionals who deal with hypertension (specialists, internists, primary care physicians) and public health workers. We believe that our patients benefit from robust scientific data that are based on well conducted clinical trials. We also believe that basic sciences are the foundations on which we build our knowledge of clinical conditions and their management. Towards this end, although we are primarily a clinical based journal, we also welcome suitable basic sciences studies that promote our understanding of human hypertension.
The journal aims to perform the dual role of increasing knowledge in the field of high blood pressure as well as improving the standard of care of patients. The editors will consider for publication all suitable papers dealing directly or indirectly with clinical aspects of hypertension, including but not limited to epidemiology, pathophysiology, therapeutics and basic sciences involving human subjects or tissues. We also consider papers from all specialties such as ophthalmology, cardiology, nephrology, obstetrics and stroke medicine that deal with the various aspects of hypertension and its complications.
 求助内容:
求助内容: 应助结果提醒方式:
应助结果提醒方式:


