19项前瞻性2期和3期试验中DLBCL患者中枢神经系统复发的识别、风险因素和临床过程--LYSA和GLA/DSHNHL合作项目
IF 12.8
1区 医学
Q1 HEMATOLOGY
引用次数: 0
摘要
对于弥漫大 B 细胞淋巴瘤(DLBCL)患者来说,中枢神经系统(CNS)的进展或复发仍然罕见,但大多是致命的。在对19项德国和法国前瞻性2/3期试验中接受治疗的5189名患者进行的回顾性分析中,我们发现159名患者出现了中枢神经系统事件(复发:62%,进展:38%)。脑内、脑膜、椎管内或合并受累的患者比例分别为 44%、31%、3% 和 22%。在 155 例可评估的患者中,62 例(40%)同时出现全身进展/复发。82%的中枢神经系统事件发生在纳入研究或随机分配后两年内。87%的患者出现中枢神经系统以外的结节外受累。患者的预后普遍较差,中位总生存期(OS)为3.4个月(95% CI为2.9-4.2),2年OS为15%(10-22%)。中枢神经系统事件发生的部位或时间点不同,结果也不尽相同。发生孤立中枢神经系统事件的患者的 OS 明显更好(p = 0.023)。25名患者接受了自体或异体干细胞移植,3年生存率为36%(20-66%)。这项包括5000多名DLBCL患者的大型研究强调,改善中枢神经系统复发的DLBCL患者预后的医疗需求尚未得到满足。本文章由计算机程序翻译,如有差异,请以英文原文为准。
Identification, risk factors, and clinical course of CNS relapse in DLBCL patients across 19 prospective phase 2 and 3 trials—a LYSA and GLA/ DSHNHL collaboration
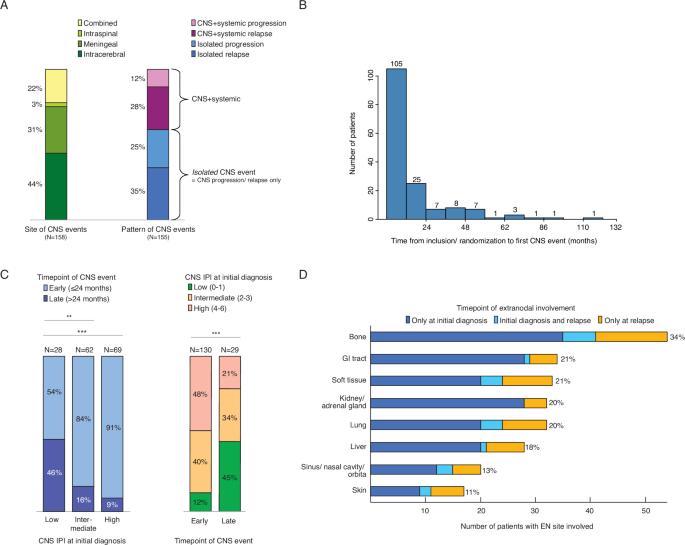
Progression or relapse in the central nervous system (CNS) remains a rare but mostly fatal event for patients with diffuse large B-cell lymphoma (DLBCL). In a retrospective analysis of 5189 patients treated within 19 prospective German and French phase 2/3 trials, we identified 159 patients experiencing a CNS event (relapse: 62%, progression: 38%). Intracerebral, meningeal, intraspinal, or combined involvement was reported in 44%, 31%, 3%, and 22% of patients, respectively. 62 of 155 evaluable patients (40%) showed concurrent systemic progression/ relapse. 82% of all CNS events occurred within two years after study inclusion or randomization. 87% of patients showed extranodal involvement outside the CNS. Patients generally had poor outcomes with a median overall survival (OS) of 3.4 months (95% CI 2.9–4.2) and a 2-year OS of 15% (10–22%). Outcomes did not differ depending on the site or time point of CNS events. Patients with isolated CNS events demonstrated significantly better OS (p = 0.023). Twenty-five patients were consolidated with autologous or allogeneic stem cell transplantation and achieved a 3-year OS of 36% (20–66%). This large study including more than 5000 DLBCL patients highlights the unmet medical need to improve the outcome of DLBCL patients suffering from CNS relapse.
求助全文
通过发布文献求助,成功后即可免费获取论文全文。
去求助
来源期刊

Leukemia
医学-血液学
CiteScore
18.10
自引率
3.50%
发文量
270
审稿时长
3-6 weeks
期刊介绍:
Title: Leukemia
Journal Overview:
Publishes high-quality, peer-reviewed research
Covers all aspects of research and treatment of leukemia and allied diseases
Includes studies of normal hemopoiesis due to comparative relevance
Topics of Interest:
Oncogenes
Growth factors
Stem cells
Leukemia genomics
Cell cycle
Signal transduction
Molecular targets for therapy
And more
Content Types:
Original research articles
Reviews
Letters
Correspondence
Comments elaborating on significant advances and covering topical issues
 求助内容:
求助内容: 应助结果提醒方式:
应助结果提醒方式:


