蛋白质组分析发现 ACSS2 有助于急性髓性白血病的代谢支持。
IF 4.8
3区 医学
Q1 BIOTECHNOLOGY & APPLIED MICROBIOLOGY
引用次数: 0
摘要
急性髓性白血病(AML)是一种异质性疾病,以癌基因的基因组畸变、细胞遗传学异常和表观遗传学异常为特征。近 50% 的急性髓细胞白血病病例在接受目前的治疗后会复发。治疗耐药性的一个主要来源是间质基质与白血病细胞的相互作用导致的治疗保护。我们的目的是确定白血病细胞间质保护过程中所涉及的促生存/抗凋亡蛋白网络。对培养的原发性急性髓细胞性白血病(n = 14)与 Hs5 基质细胞系进行蛋白质组分析,发现了能量代谢蛋白的上调。接下来,我们用表观遗传药物库调节了基质诱导的耐药性,结果发现组蛋白去乙酰化酶抑制剂(HDACi)与其他表观遗传修饰化合物相比,能减少细胞凋亡。对这种效应的定量磷酸蛋白组探测进一步揭示了新陈代谢丰富的磷酸蛋白组,包括与未处理的单一培养物相比,在白血病-基质 HDACi 处理的共培养物中乙酰辅酶 A 合成酶(ACSS2,S30)显著上调。为了验证这些发现,我们发现 ACSS2 底物乙酸酯可促进白血病细胞增殖,敲除白血病细胞中的 ACSS2 可抑制白血病细胞增殖,而敲除基质中的 ACSS2 则会损害白血病细胞的代谢能力。最后,我们发现 ACSS1/ACSS2 高表达急性髓细胞性白血病亚型与总生存率低相关。总之,这项研究揭示了白血病基质磷酸蛋白组,强调了 ACSS2 在介导急性髓细胞性白血病生长和耐药性方面的作用。本文章由计算机程序翻译,如有差异,请以英文原文为准。
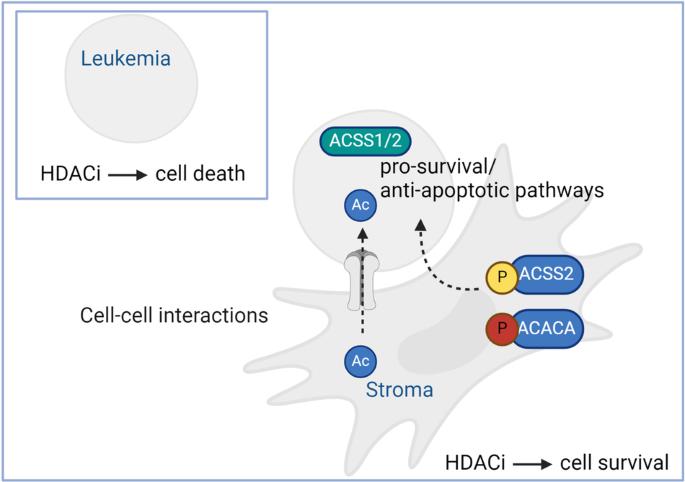
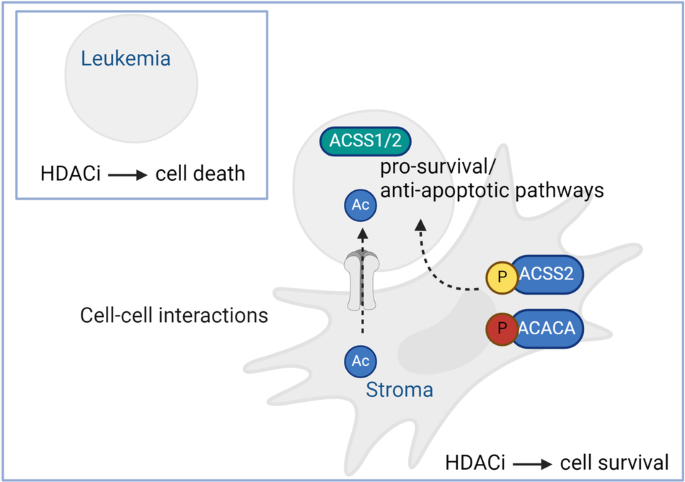
Proteomic profiling reveals ACSS2 facilitating metabolic support in acute myeloid leukemia
Acute myeloid leukemia (AML) is a heterogeneous disease characterized by genomic aberrations in oncogenes, cytogenetic abnormalities, and an aberrant epigenetic landscape. Nearly 50% of AML cases will relapse with current treatment. A major source of therapy resistance is the interaction of mesenchymal stroma with leukemic cells resulting in therapeutic protection. We aimed to determine pro-survival/anti-apoptotic protein networks involved in the stroma protection of leukemic cells. Proteomic profiling of cultured primary AML (n = 14) with Hs5 stroma cell line uncovered an up-regulation of energy-favorable metabolic proteins. Next, we modulated stroma-induced drug resistance with an epigenetic drug library, resulting in reduced apoptosis with histone deacetylase inhibitor (HDACi) treatment versus other epigenetic modifying compounds. Quantitative phosphoproteomic probing of this effect further revealed a metabolic-enriched phosphoproteome including significant up-regulation of acetyl-coenzyme A synthetase (ACSS2, S30) in leukemia-stroma HDACi treated cocultures compared with untreated monocultures. Validating these findings, we show ACSS2 substrate, acetate, promotes leukemic proliferation, ACSS2 knockout in leukemia cells inhibits leukemic proliferation and ACSS2 knockout in the stroma impairs leukemic metabolic fitness. Finally, we identify ACSS1/ACSS2-high expression AML subtype correlating with poor overall survival. Collectively, this study uncovers the leukemia-stroma phosphoproteome emphasizing a role for ACSS2 in mediating AML growth and drug resistance.
求助全文
通过发布文献求助,成功后即可免费获取论文全文。
去求助
来源期刊

Cancer gene therapy
医学-生物工程与应用微生物
CiteScore
10.20
自引率
0.00%
发文量
150
审稿时长
4-8 weeks
期刊介绍:
Cancer Gene Therapy is the essential gene and cellular therapy resource for cancer researchers and clinicians, keeping readers up to date with the latest developments in gene and cellular therapies for cancer. The journal publishes original laboratory and clinical research papers, case reports and review articles. Publication topics include RNAi approaches, drug resistance, hematopoietic progenitor cell gene transfer, cancer stem cells, cellular therapies, homologous recombination, ribozyme technology, antisense technology, tumor immunotherapy and tumor suppressors, translational research, cancer therapy, gene delivery systems (viral and non-viral), anti-gene therapy (antisense, siRNA & ribozymes), apoptosis; mechanisms and therapies, vaccine development, immunology and immunotherapy, DNA synthesis and repair.
Cancer Gene Therapy publishes the results of laboratory investigations, preclinical studies, and clinical trials in the field of gene transfer/gene therapy and cellular therapies as applied to cancer research. Types of articles published include original research articles; case reports; brief communications; review articles in the main fields of drug resistance/sensitivity, gene therapy, cellular therapy, tumor suppressor and anti-oncogene therapy, cytokine/tumor immunotherapy, etc.; industry perspectives; and letters to the editor.
 求助内容:
求助内容: 应助结果提醒方式:
应助结果提醒方式:


