中国2型糖尿病患者中性粒细胞与淋巴细胞比率和血小板与淋巴细胞比率与糖尿病肾病的关系:一项横断面研究
IF 2.3
3区 医学
Q2 HEALTH CARE SCIENCES & SERVICES
引用次数: 3
摘要
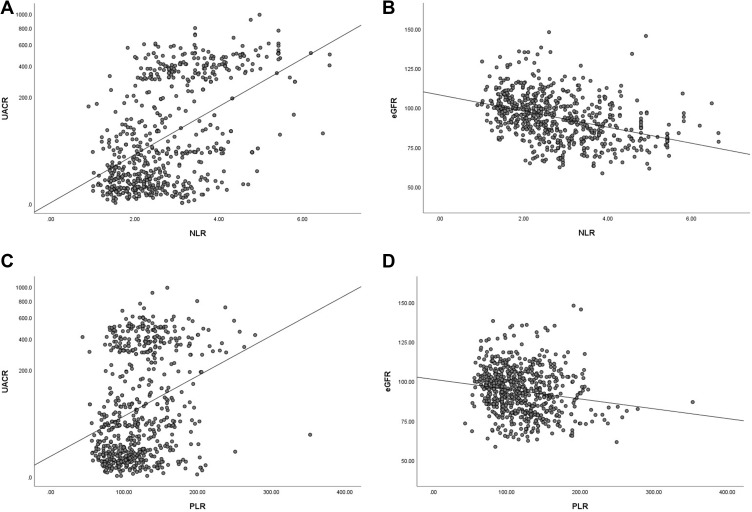
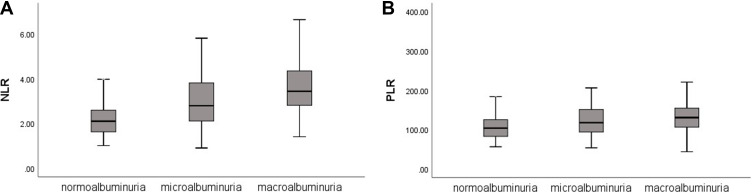
目的:中性粒细胞与淋巴细胞比值(NLR)和血小板与淋巴细胞比值(PLR)在多种疾病中得到了广泛的研究。然而,关于它们与糖尿病肾病(DKD)关系的研究有限。我们的研究目的是探讨这两个指标与中国2型糖尿病患者肾功能之间的关系,并评估它们是否可以作为DKD的预测指标。方法:本横断面研究纳入655例中国2型糖尿病患者。根据尿白蛋白与肌酐比值(UACR)将受试者分为三组。分析各组NLR、PLR的差异及其与肾功能的相关性。采用Logistic回归分析分析DKD的独立危险因素,采用受试者工作特征(ROC)曲线评估NLR和PLR对疾病的预测价值。结果:三组患者NLR、PLR差异有统计学意义,且随蛋白尿水平升高而升高。Pearson相关分析显示NLR和PLR与UACR呈正相关,与肾小球滤过率(glomerular filtration rate, eGFR)估测值呈负相关(ppppp)。结论:中国2型糖尿病患者NLR和PLR与肾功能密切相关,高NLR和PLR值可作为DKD的预测指标。本文章由计算机程序翻译,如有差异,请以英文原文为准。
Association of Neutrophil-to-Lymphocyte Ratio and Platelet-to-Lymphocyte Ratio with Diabetic Kidney Disease in Chinese Patients with Type 2 Diabetes: A Cross-Sectional Study.
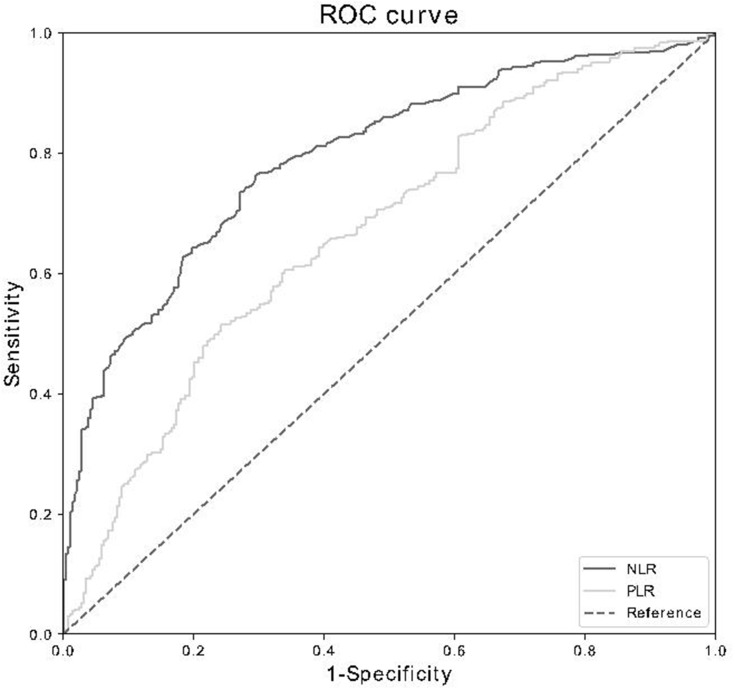
Purpose The neutrophil-to-lymphocyte ratio (NLR) and platelet-to-lymphocyte ratio (PLR) have been extensively studied in a variety of diseases. However, research on their relationship with diabetic kidney disease (DKD) is limited. The aim of our study was to investigate the association between these two indicators and renal function in Chinese patients with type 2 diabetes and assess whether they can serve as predictors of DKD. Methods This cross-sectional study enrolled 655 Chinese patients with type 2 diabetes. Subjects were divided into three groups according to the urinary albumin-to-creatinine ratio (UACR). The differences in the NLR and PLR among the groups and their correlation with renal function were analyzed. Logistic regression analysis was used to analyze independent risk factors for DKD, and receiver operating characteristic (ROC) curves were used to assess the predictive values of the NLR and PLR for the disease. Results The NLR and PLR were significantly different among the three groups, and they increased with increasing levels of albuminuria. Pearson’s correlation analysis showed that the NLR and PLR were positively correlated with the UACR but negatively correlated with the estimated glomerular filtration rate (eGFR) (p<0.001). Logistic regression analysis showed that these two indicators were independent risk factors for DKD (p<0.001). The results of ROC curve analysis suggested that the NLR (AUC=0.794; 95% CI, 0.760–0.827; p<0.001) and PLR (AUC=0.665; 95% CI, 0.623–0.706, p<0.001) had important diagnostic value for DKD. Conclusion The NLR and PLR were closely associated with renal function among Chinese patients with type 2 diabetes, and high NLR and PLR values may serve as predictors of DKD.
求助全文
通过发布文献求助,成功后即可免费获取论文全文。
去求助
来源期刊

Therapeutics and Clinical Risk Management
HEALTH CARE SCIENCES & SERVICES-
CiteScore
4.80
自引率
3.60%
发文量
139
审稿时长
16 weeks
期刊介绍:
Therapeutics and Clinical Risk Management is an international, peer-reviewed journal of clinical therapeutics and risk management, focusing on concise rapid reporting of clinical studies in all therapeutic areas, outcomes, safety, and programs for the effective, safe, and sustained use of medicines, therapeutic and surgical interventions in all clinical areas.
The journal welcomes submissions covering original research, clinical and epidemiological studies, reviews, guidelines, expert opinion and commentary. The journal will consider case reports but only if they make a valuable and original contribution to the literature.
As of 18th March 2019, Therapeutics and Clinical Risk Management will no longer consider meta-analyses for publication.
The journal does not accept study protocols, animal-based or cell line-based studies.
 求助内容:
求助内容: 应助结果提醒方式:
应助结果提醒方式:


