Livestream, group movement program for people living with cognitive impairment and care partners: A randomized clinical trial
Abstract
INTRODUCTION
There are few widely-available, evidence-based options to support quality of life (QOL) for people living with Alzheimer's disease and related dementias.
METHODS
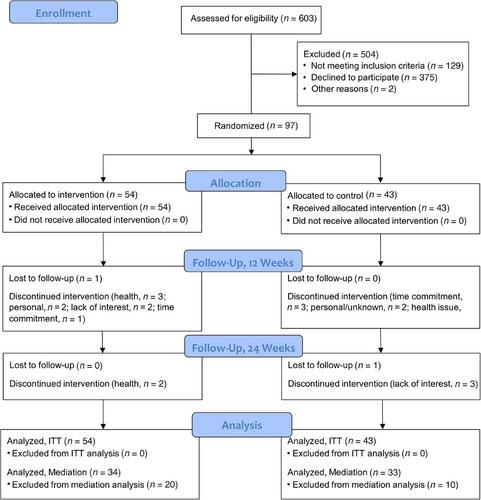
We performed a randomized, controlled trial with a Waitlist control group to determine whether an online, livestream, mind-body, group movement program (Moving Together, 1 hour, 2 days/week, 12 weeks) improves QOL in people with cognitive impairment (PWCI) or care partners (CPs) and explore mechanisms of action. The primary outcome for both participants was self-reported QOL. Secondary outcomes and potential mediators included mobility, isolation, well-being, cognitive function, and sleep in PWCI and burden, positive emotions, caregiver self-efficacy, stress management, and sleep in CPs. Blinded assessors collected outcome data at baseline, 12, and 24 weeks. We assessed adverse events including falls through monthly check-in surveys and collected qualitative data through evaluation surveys. Intention-to-treat analyses used linear mixed models to compare mean change over time between groups and calculated standardized effect sizes (ESs).
RESULTS
Ninety-seven dyads enrolled (PWCI: age 76 ± 11 years, 43% female, 80% non-Hispanic White; CPs: age 66 ± 12 years, 78% female, 71% non-Hispanic White); 15% withdrew before 12 weeks and 22% before 24 weeks. PWCI self-reported significantly better QOL from baseline to 12 weeks in the Moving Together group compared to the Waitlist group (ES = 0.474, p = 0.048) and CPs self-reported improved ability to manage stress (ES = 0.484, p = 0.021). Improvements in participant self-reported QOL were mediated by improvements in their self-reported well-being and CP-reported ability to manage stress. Results were similar when the Waitlist group participated in the program (QOL ES = 0.663, p = 0.006; stress management ES = 0.742, p = 0.002) and were supported by qualitative data. Exploratory analyses suggested possible fall reduction in PWCI. There were no study-related serious adverse events.
DISCUSSION
Online programs such as Moving Together offer a scalable strategy for supporting high QOL for PWCI and helping CPs manage stress.
TRIAL REGISTRATION
ClinicalTrials.gov NCT04621448
Highlights
- The approval of new medications that slow cognitive decline in people living with Alzheimer's disease and related disorders (ADRD) has raised hope and excitement. However, these medications do not appear to impact quality of life, which is often considered by patients and care partners to be the most important outcome.
- In this randomized clinical trial, we found that an evidence-based, online, livestream, mind-body, group movement program significantly and meaningfully improves self-rated quality of life in people with ADRD and helps care partners manage stress. Mediation analyses revealed that the key drivers of improvements in participants’ quality of life were improvements in their feelings of well-being and care partners’ ability to manage stress. Exploratory analyses also suggested a 30% reduction in falls.
- These results are important because they suggest that an online program, which is available now and can be performed by people from the comfort of home or other location of choice, could be recommended as a complement or alternative to new therapies to help maximize quality of life for people living with ADRD and their care partners.

 求助内容:
求助内容: 应助结果提醒方式:
应助结果提醒方式:


