Injection network drivers of HIV prevention service utilization among people who inject drugs: results of a community-based sociometric network cohort in New Delhi, India
Abstract
Introduction
Injection drug networks may influence their network members’ health-seeking behaviours. Using data from a sociometric injecting partner network of people who inject drugs (PWID) in New Delhi, India, we assessed the role of injecting partner (alter) behaviours on individual engagement in HIV prevention services.
Methods
We enumerated injecting partner linkages among 2512 PWID using coupon referrals and biometric data from November 2017 to March 2020. Participants completed interviewer-administered questionnaires and provided information on injection behaviours, injecting partners, HIV/hepatitis C (HCV) testing and service engagement. Multilevel multiple-membership models (MMMM) evaluated individual PWID HIV testing, medication for opioid use disorder (MOUD) and syringe service engagement as a function of alter attributes, accounting for membership across multiple ego-networks. Logistic regression models assessed parallel associations among socially proximal injecting peers, defined as PWID ≤3 path length from ego.
Results
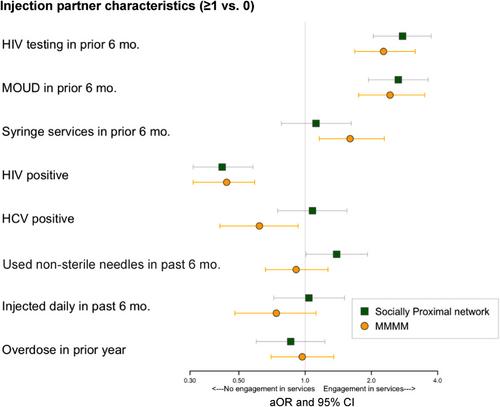
Median age was 26 years; 99% were male. PWID had median 2 injecting partners and 8 socially proximal peers; 14% reported HIV testing, 33% accessed MOUD and 13% used syringe services 6 months prior. In MMMM analyses, PWID with ≥1 versus 0 injecting partners who received HIV testing were significantly more likely to report HIV testing (adjusted odds ratio [aOR]: 2.27, 95% confidence interval [CI]: 1.68–3.16), MOUD (aOR: 1.99, 95% CI: 1.60–2.53) and syringe service use (aOR: 1.66, 95% CI: 1.21–2.39). We observed similar findings for individual MOUD and syringe service use. Having ≥1 versus 0 HIV-positive partners was associated with decreased HIV testing and MOUD but increased syringe service use (aOR: 1.54, 95% CI: 1.09–2.17). PWID with ≥1 versus 0 socially proximal peers who used non-sterile injection equipment reported increased HIV testing (aOR: 1.39, 95% CI: 1.01–1.92), MOUD (aOR: 1.40, 95% CI: 1.10–1.77) and syringe service use (aOR: 1.82, 95% CI: 1.23–2.68).
Conclusions
We found differential associative relationships between individual HIV prevention service engagement and the health or risk behaviours of direct and indirect alters. Characterizing network exposure beyond direct injecting partnerships provided important context on possible mechanisms of behavioural influence. Findings could be leveraged to design peer-based interventions that promote network diffusion of health-seeking behaviours.

| 公司名称 | 产品信息 | 采购帮参考价格 |
|---|
 求助内容:
求助内容: 应助结果提醒方式:
应助结果提醒方式:


